Pigmentation
Unraveling the Mysteries of Pigmentation: Understanding Spots, Patches, and Your Unique Skin Tone

Our skin, the largest organ of our body, is a complex canvas painted with a spectrum of hues. This beautiful diversity is largely determined by melanin, a pigment produced by specialized cells called melanocytes. However, sometimes these melanocytes can go into overdrive or underperform, leading to changes in our skin tone that we commonly refer to as pigmentation.
From sunspots to melasma, understanding the different types of pigmentation, their causes, and the available management strategies is key to achieving healthy, even-toned skin and feeling confident in your own complexion.
What Exactly is Pigmentation?
At its core, pigmentation refers to the coloring of the skin. When this coloring becomes uneven, resulting in darker or lighter patches compared to your natural skin tone, it’s considered a pigmentation disorder. These changes can be localized to small spots or cover larger areas of the body.
Common Types of Pigmentation and Their Culprits:
Let’s explore some of the most prevalent forms of pigmentation:
Hyperpigmentation (Darkening of Skin): This occurs when there’s an excess production of melanin. Common types include:
- Sunspots (Solar Lentigines): These flat, brown spots are a direct result of prolonged sun exposure over time. They often appear on sun-exposed areas like the face, hands, and décolletage.
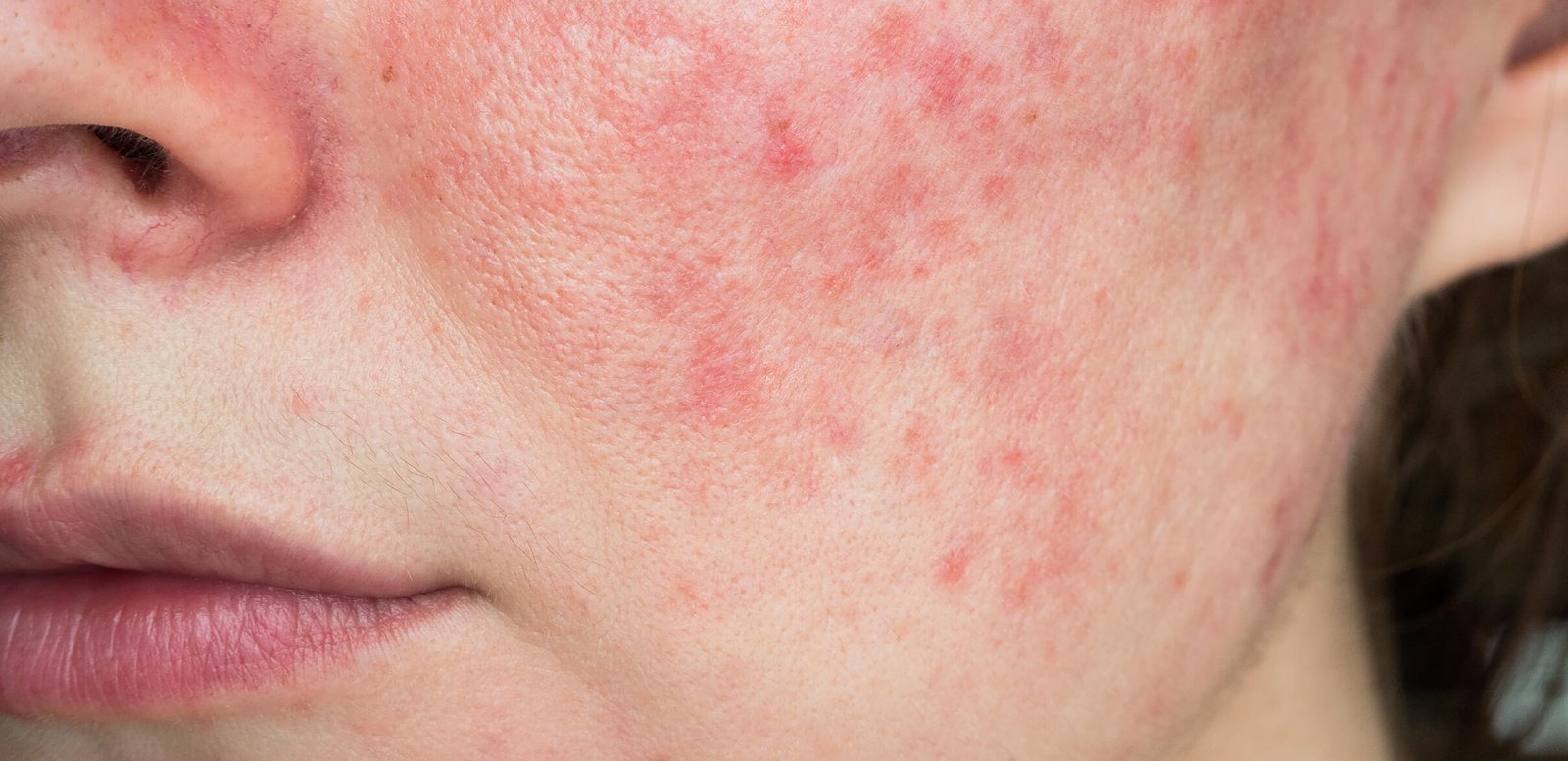
- Post-Inflammatory Hyperpigmentation (PIH): This darkening of the skin occurs after an injury or inflammation, such as acne breakouts, eczema, insect bites, or burns. The pigment lingers even after the initial skin issue has resolved.
- Melasma: As discussed in a previous blog, this condition presents as symmetrical brown or grayish-brown patches, often on the face (cheeks, forehead, upper lip). Hormonal fluctuations (pregnancy, birth control), sun exposure, and genetics are key contributing factors.
- Freckles (Ephelides): These small, flat, brown spots are also triggered by sun exposure and are more common in individuals with lighter skin and hair. They tend to darken in the summer and fade in the winter.
Hypopigmentation (Lightening of Skin): This occurs due to a decrease in melanin production. Common types include:
- Vitiligo: This autoimmune condition causes the destruction of melanocytes, resulting in smooth, white patches of skin that can appear anywhere on the body.
- Post-Inflammatory Hypopigmentation: Similar to hyperpigmentation, skin inflammation can sometimes lead to a loss of pigment in the affected area.
- Pityriasis Alba: This common childhood condition presents as scaly, pale patches, often on the face, neck, and upper arms. Its exact cause is unknown but may be related to mild eczema.
At its core, pigmentation refers to the coloring of the skin. When this coloring becomes uneven, resulting in darker or lighter patches compared to your natural skin tone, it’s considered a pigmentation disorder. These changes can be localized to small spots or cover larger areas of the body.
Understanding the Causes: Unmasking the Triggers
Several factors can contribute to the development of pigmentation disorders:
- Sun Exposure: The number one culprit for many forms of hyperpigmentation. UV radiation stimulates melanocytes to produce more melanin as a protective mechanism.
- Hormonal Changes: Fluctuations in hormones, particularly estrogen and progesterone, can trigger melasma.
- Inflammation and Injury: Skin trauma can lead to both hyper- and hypopigmentation as the skin heals.
- Genetics: A predisposition to certain pigmentation conditions, like freckles and melasma, can be inherited.
- Medications: Some medications can increase photosensitivity, making the skin more prone to pigmentation changes with sun exposure.
- Underlying Medical Conditions: Certain autoimmune diseases (like vitiligo) can directly affect melanin production.
